

About 800,000 Canadian adults have Barrett’s esophagus.8 Barrett’s esophagus can increase a person’s risk of cancer of the esophagus by 50 times or more.4,6,7,9

Barrett’s esophagus is a disease affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth to the stomach. It is caused by injury to the esophagus from the chronic backwash of stomach contents, like acid and enzymes, that occurs with abnormal reflux.
People with Barrett’s esophagus may not have any symptoms.10 However, chronic heartburn, difficulty swallowing, nausea, chest pain and other symptoms of GERD may indicate a need for further testing. It is estimated that up to 15% of the people who have chronic acid reflux — those in high risk groups including chronic GERD, Caucasian, male, over age 50 — may develop Barrett’s esophagus.11
In addition to suffering from chronic heartburn, other factors that may put a person at risk for Barrett’s esophagus include:13
Obesity
Caucasian ethnicity
Family history
Male gender
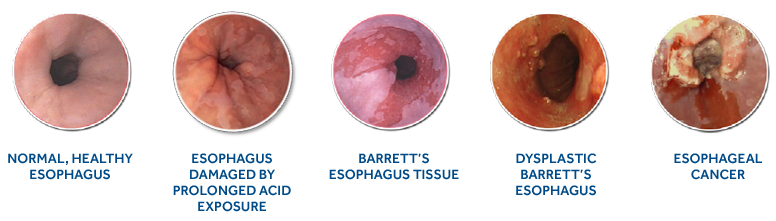
Once a person has Barrett’s esophagus, it may continually progress to more serious stages, potentially resulting in esophageal adenocarcinoma, a type of esophageal cancer. There are three stages of Barrett’s esophagus and range from the least serious (intestinal metaplasia without dysplasia) to the most serious (high-grade dysplasia). Dysplasia refers to the abnormalities of tissue or a cell that make it more cancer-like and disorganized. The presence of dysplasia is not considered cancer, but may increase the risk of developing cancer.3,14 Each stage of Barrett’s esophagus is distinguished by the following:
The normal epithelium (lining) of the esophagus is replaced with a type of epithelium resembling that found in the intestine.
Cells appear abnormal when viewed under a microscope and represent a very early stage of pre-cancer of the esophagus.
Cancer occurs when the abnormal cells involved in Barrett’s esophagus have rapid and uncontrolled growth and invade the deeper layers of your esophagus. This is called cancer of the esophagus, or esophageal adenocarcinoma (EAC). The cancer can also spread beyond the esophagus.
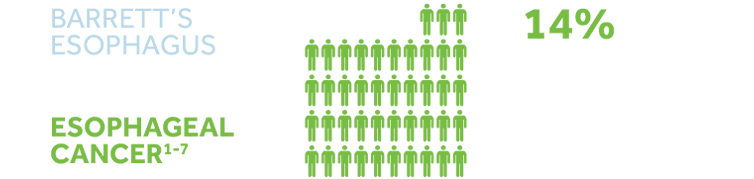
Although still considered rare, EAC one of the most rapidly rising cancer in Canada.14,15 Patients with Barrett’s esophagus are 30 to 125 times more at risk of developing EAC than patients without the condition.16 Roughly 14% of patients survive at least five years after the diagnosis of esophageal cancer.15
The good news is that there is treatment available. Treatment of Barrett’s esophagus has been shown to reduce the risk of progression to high-grade dysplasia and esophageal adenocarcinoma.17,18
Talk to your physician to learn if you or a loved one are at risk for Barrett’s esophagus.
References:
1. Fedorak et al, Canadian Digestive Health Foundation Public Impact Series: Gastroesophageal reflux disease in Canada: Incidence, prevalence, and direct and indirect economic impact, Can J Gastrolenterol 2010; 24(7):431-434
2. Vakil et al, The Montreal Definition and Classificatio of Gastroesophegeal Reflux Disease: A Global Evidence-Based Consensus, Am J Gastroenterol 2006; 101:1900-1920
3. American Society for Gastrointestinal Endoscopy, https://www.asge.org/home/for-patients/patient-information/understanding-gerd-barrett-39-s
4. Vaezi M, Zehrai A, Yuksel E, Testing for refractory gastroesophageal reflux disease, ASGE Leading Edge, 2012 Vol 2, No 2, 1-13, American Society Gastroenterology Esdoscopy, Page 1-2
5. Gilbert EW et al. Barrett’s esophagus: a review of the literature. J Gastrointest Surg 2011;15:708-1
6. Pohl H, Welch G et al. The role of over diagnosis and reclassification in the marked increase of esophageal adenocarcinoma incidence. J Natl Cancer Inst 2005;97:142-6
7. SEER Cancer Statistics Factsheets: Esophageal Cancer. National Cancer Institute. Bethesda, MD,http://seer.cancer.gov/statfacts/html/esoph.html
8. Canadian Digestive Health Foundation; http://cdhf.ca
9. Wani S, Falk G, Hall M, Gaddam S, Wang A, Gupta N, et al. Patients with nondysplastic Barrett’s esophagus have low risks for developing dysplasia or esophageal adenocarcinoma. Clin Gastroenterol Hepatol. 2011;9(3):220-7.
10. Shaheen NJ, Richter JE. Barrett’s oesophagus. Lancet. 2009;373(9666):850-61.
11. Gilbert EW et al. Barrett’s esophagus: a review of the literature. J Gastrointest Surg 2011;15:708-1
12. Canadian Cancer Society, Canadian Cancer Statistics 2017, Special topic: Pancreatic cancer
13. Spechler SJ, Souza RF. Barrett’s esophagus. NEJM. 2014;371:836-45.
14. Reid BJ, Weinstein WM. Barrett’s esophagus and adenocarcinoma. Gastroenterology Clinics of North America. 1987;38:477-92.
15. Canadian Cancer Society, Canadian Cancer Statistics 2017, Special topic: Pancreatic cancer
16. Eisen GM. Ablation therapy for Barrett's esophagus. Gastrointestinal Endosc. 2003;58:760-9.
17. Phoa KN, van Vilsteren FG, Weusten BL, Bisschops R, Schoon EJ, Ragunath K, et al. Radiofrequency ablation vs endoscopic surveillance for patients with Barrett esophagus and low-grade dysplasia: a randomized clinical trial. JAMA. 2014;311(12)1209-17. doi:10.1001/jama.2014.2511.
18. Wolf WA, Pasricha S, Cotton C, Li N, Triadafilopoulos G, Raman Muthusamy V, et al. Incidence of Esophageal Adenocarcinoma and Causes of Mortality After Radiofrequency Ablation of Barrett’s Esophagus. Gastroenterology. 2015;149(7):1752-1761.